How low wages and high rent helped Covid spread from a wedding in Kent to nearly 300
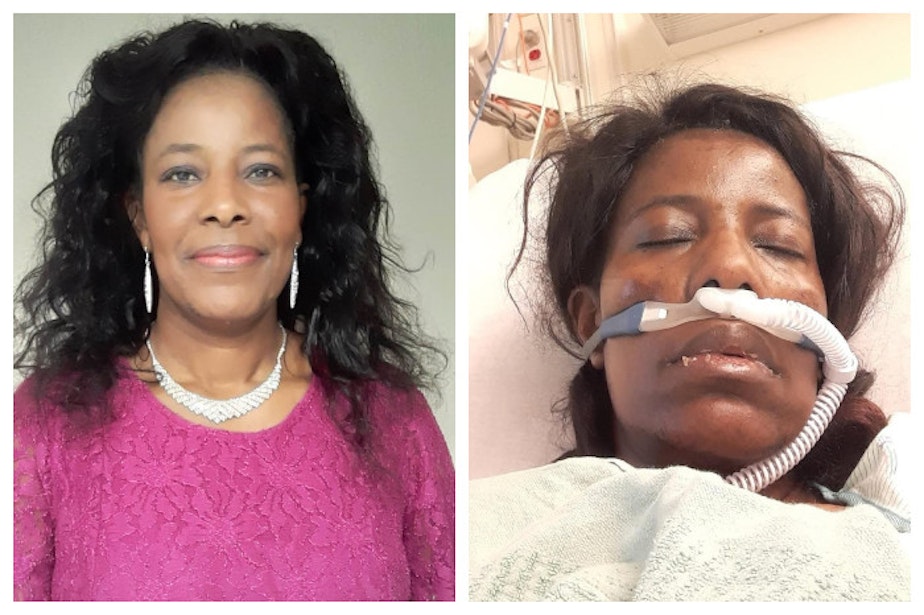
It was July 2020, and the sky was a brilliant blue.
The guests assembled inside Christ the King Anglican Church in Kent, Washington, for what would be a very fun wedding — and a coronavirus superspreader event.
At the altar, a group stood close together. Church leaders sang a prayer of protection for the new couple. Their voices joined in unison and their masks were pulled down to their chins, exposing their noses and mouths.
A few small windows were open.
Zipporah Maina was there; her official title for the day was “Cake Matron,” and she helped the couple cut the cake.
As weddings go, it was fantastic.
“In my culture people celebrate weddings a lot,” said Maina, who is from Kenya originally, like the couple and their guests. “There was a lot of dancing, there was a lot of singing, there was a lot of joy.”
Sponsored
At least 10 people got Covid from the wedding, including Maina and the groom.
From there, the virus infected close to 300 people in all and caused outbreaks at over 40 healthcare facilities. Fifteen people died.
The virus benefited not only from the large gathering, but from layers of economic and social vulnerability that created great conditions for spread. Improper masking and asymptomatic spread played a part – and so did low wages, high rent, and the stigma of testing positive.
No one knows how many more outbreaks there were like this that went undetected and uninvestigated. As KUOW has reported, the pandemic has so overwhelmed public health resources, investigators simply cannot follow up on every lead.
A video of the wedding was posted publicly to YouTube, and it shows conditions that are known to spread Covid. For example, at the reception, around 70 people ate dinner and made toasts with their masks off.
Sponsored
“Where we were sitting, I recall, shoulder to shoulder,” Maina said. “If I stretched my arm out, definitely I would touch the person next to me.”
Maina's symptoms exhibited less than a week after the wedding.
"Every time I would cough my chest would feel so much pain,” she said.
Within days, she was in the intensive care unit with pneumonia from Covid.
Maina got worse and worse.
Sponsored
A few weeks after she was admitted to the hospital, she sat up in bed for the first time.
She sent friends a video, the hiss of hospital equipment in the background nearly swallowing her breathless, strained voice.
“Just keep praying for me,” she said. “I love you so much, and I miss you.”
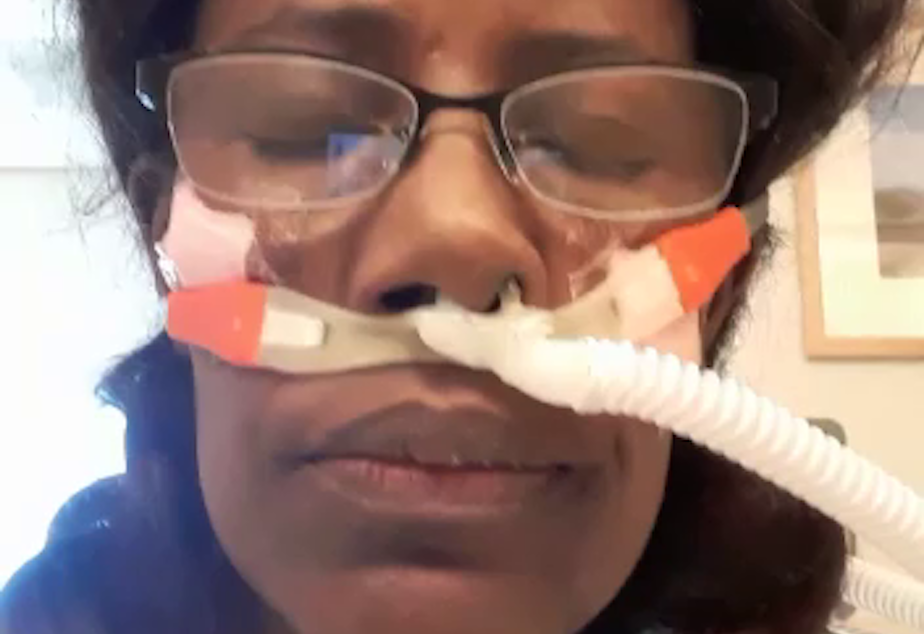
 1 min
Zipporah Maina, who got Covid-19 from a July 2020 wedding, sent this video to friends the first day she could sit up in bed after being admitted to the hospital.
1 min
Zipporah Maina, who got Covid-19 from a July 2020 wedding, sent this video to friends the first day she could sit up in bed after being admitted to the hospital.
Meanwhile, the virus continued on its path. Many of the people who got infected at the wedding worked in healthcare facilities such as group homes for adults with intellectual and developmental disabilities. Public health investigators traced the virus from six attendees to outbreaks at their jobs.
Sponsored
James Lewis oversaw the investigation for Public Health – Seattle & King County. He said one reason for the outbreak goes back to something really tricky about Covid.
“There’s a lot of asymptomatic spread,” Lewis said. “You go to a wedding, and you don't know that you contract Covid. And so you go to work as usual.”
Bethesda Lutheran Communities was among the workplaces that got hit.
Local director, Zola Sheehan, was the first person to help public health link the outbreak to the wedding. She offhandedly mentioned it on the phone one day, she said, and it allowed investigators to link together seemingly unconnected outbreaks.
And here’s something really important to understand about this outbreak.
Sponsored
Staff at her agency said they were exposed to Covid at their other jobs. Caregivers for adults with disabilities often have two or three jobs. They have to, because the pay is so low. Sheehan said it’s an industry-wide problem – there’s just not enough state funding.
That’s why Sheehan was not angry with the staff for bringing Covid into the facility.
"I was angry that the industry required staff to have more than one job,” she said. “But when you get right down to it, you do what you have to do.”
That staffing model meant that when one employee was out sick, two or three jobs needed to find a replacement. At one point, Bethesda Lutheran was so short-staffed that Sheehan started making contingency plans if only a handful of employees could work.
"We were starting to talk to churches to see if we could, during the day, just move all of our people together into one location, like a friendship hall,” she said.
Others quarantined on the job, living with the residents they supported.
That’s what caregiver Joseph Kiurire did.
Kiurire has two jobs and works 12-hour shifts, six days a week so he can pay bills and save money to become a nurse.
When cases flared last summer at one of his work places, Integrated Living Services, Kiurire stayed for more than a week caring for one resident, David Evans, a 65 year-old man with autism who cannot speak.
Kiurire slept on an air mattress on the living room floor. He didn’t really care about that; he cared about advocating for Evans and the other residents.
“Because I myself, I can take care of myself. What about them?” he said.
Kiurire wore protective gear and didn’t get Covid. At one point, Evans was hospitalized on a ventilator, and Kiurire visited.
“It was so emotional for me, because I have worked for him like three years,” Kiurire said.
Evans survived. The 15 other people who died in the wedding outbreak were residents of facilities that care for intellectually and developmentally disabled adults.
Kiurire heard about the wedding last July linked to the outbreak, but he did not go.
He felt the effects anyway. A dozen people at his job got Covid.
If you want to understand this outbreak, here’s one more thing to consider.
The stigma of a positive Covid case also helped the virus spread, said Joseph Emmanuel, Integrated Living Services executive director, because staff wouldn’t tell managers they had been exposed.
Emmanuel said revealing your Covid-positive status could mean losing your roommates, with whom you need to split rent, or even your entire support network.
"You’re going to be left alone. You may not be able to live. And, especially in the African community, when you can’t have a friend, where are you going to go and find somebody else?” Emmanuel said. “You don’t have a family member. Most people do not have a lot of family members here.”
That stigma was very real for Zipporah Maina, who got Covid at that wedding last July.
When she left the hospital, she needed help with everything from walking to bathing.
Maina’s family is back in Kenya – and some friends were not willing to help.
“Even after getting out of hospital after being in 40 days and recovering, people still felt like I was infectious,” she said.
Maina’s health has not recovered. She can’t cook and wash dishes at the same time, for example.
“If I'm not cautious," she said, "within a very short time, I'm tired. I want to sit down,” she said.
She's outspoken, despite the stigma.
“I don't want anybody to get this thing. It's terrible,” she said.
A few friends did help her, for which she is thankful, she said. They helped her with daily tasks she couldn’t do. Some took time off work and drove a long way to take her to doctor’s appointments.
And, the pastor of the church where that wedding took place held a major fundraiser for her medical and living expenses.
“When I look at the statistics of how many people have passed on," she said, "I just realize how blessed I am to be alive today.”




